Dental caries
Chronic destruction of dental hard tissue caused by plaque, sugar intake, inadequate oral hygiene, and related factors. Early lesions can be managed, while cavitated lesions usually require restorative treatment.
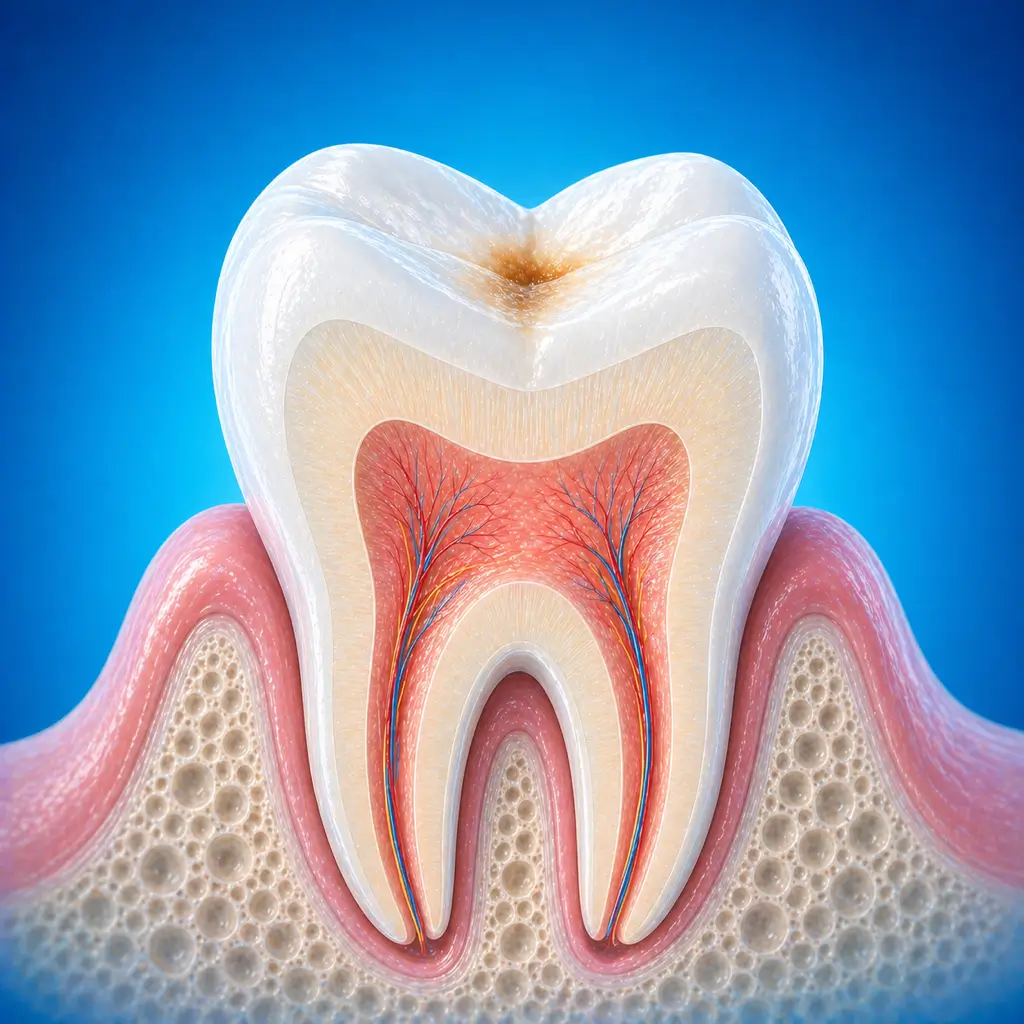
Common Symptoms
Recognizing Dental caries
Focus on the most useful decision cues first: common symptoms, the patients or situations that usually prompt review, and any signs that need faster assessment.
Common Symptoms
Signs patients often notice before evaluation
Early disease may cause no obvious discomfort, with chalky, yellow-brown, or black changes on the tooth surface
After a cavity forms, food impaction, a visible hole, tooth darkening, or tooth structure loss may occur
Pain from cold, heat, sour, or sweet stimuli usually improves after the stimulus is removed
When decay approaches the pulp, persistent pain, night pain, or pain on biting may occur
When to Seek Evaluation
Typical patients and situations that warrant review
Can occur at any age
Black spots, chalky patches, or cavities are found on teeth
Repeated food impaction or sensitivity and pain during brushing or eating
Pain from cold, heat, sour, or sweet stimuli, pain on biting, or night pain
Caries in primary teeth or young permanent teeth in children, requiring assessment of possible effects on permanent tooth development or pulp status
Treatment Approaches
Treatment Directions for Dental caries
Early enamel demineralization may be monitored with improved oral hygiene, sugar control, fluoride measures, and remineralization therapy
When a cavity or food impaction is present, tooth filling restoration is usually needed
When decay approaches or involves the pulp, pulp protection, root canal treatment, or later crown/inlay restoration may need assessment
What usually shapes the treatment plan
Clinical Assessment
Key Assessments for Dental caries
These are the main areas doctors usually review first. If you already have relevant test or imaging reports, bring them to speed up the assessment. They are helpful but not required, and the same workup can also be completed in China.
Location of decay
Depth and whether a cavity has formed
Pulp vitality and signs of irreversible pulpitis or periapical periodontitis
Interproximal caries
Risk of recurrent and multiple caries
Oral hygiene
Frequency of sugar intake
Fluoride exposure and salivary/systemic risk factors
Before You Travel
How to Prepare
Prepare previous dental treatment records and recent imaging in advance (periapical radiographs, panoramic radiographs, or CBCT, if available)
List systemic diseases, allergy history, and current medications, especially anticoagulants, antidiabetic drugs, bisphosphonates, or immunosuppressants
Keep the mouth clean on the day of the visit; follow hospital fasting instructions if surgery or sedation is involved
Planning Notes
Pre-Assessment Required
An intraoral examination is needed. Bitewing radiographs, periapical radiographs, or CBCT may be taken when necessary to assess lesion depth, interproximal caries, and periapical status. The dentist will combine pulp vitality testing, percussion, occlusal examination, and caries risk assessment to decide among observation, remineralization, filling, pulp protection, or root canal treatment.
Remote Pre-Assessment
Remote materials can only be used for preliminary triage. Diagnosis and treatment planning usually require an in-person intraoral examination and imaging assessment.
Multidisciplinary Assessment
Medical History Important
In most cases, previous medical records are not the only deciding factor, but dental imaging, treatment records, drug allergies, or chronic disease medications should still be brought to help the dentist assess the case.
Ready to Explore Treatment for Dental caries?
Let Carevia help you connect with the right specialists, compare hospitals, and plan your medical trip to China.