Tooth fracture
Fracture of tooth structure due to trauma, biting hard objects, caries, or other causes. Treatment depends on fracture depth, pulp exposure, root status, and periodontal support.
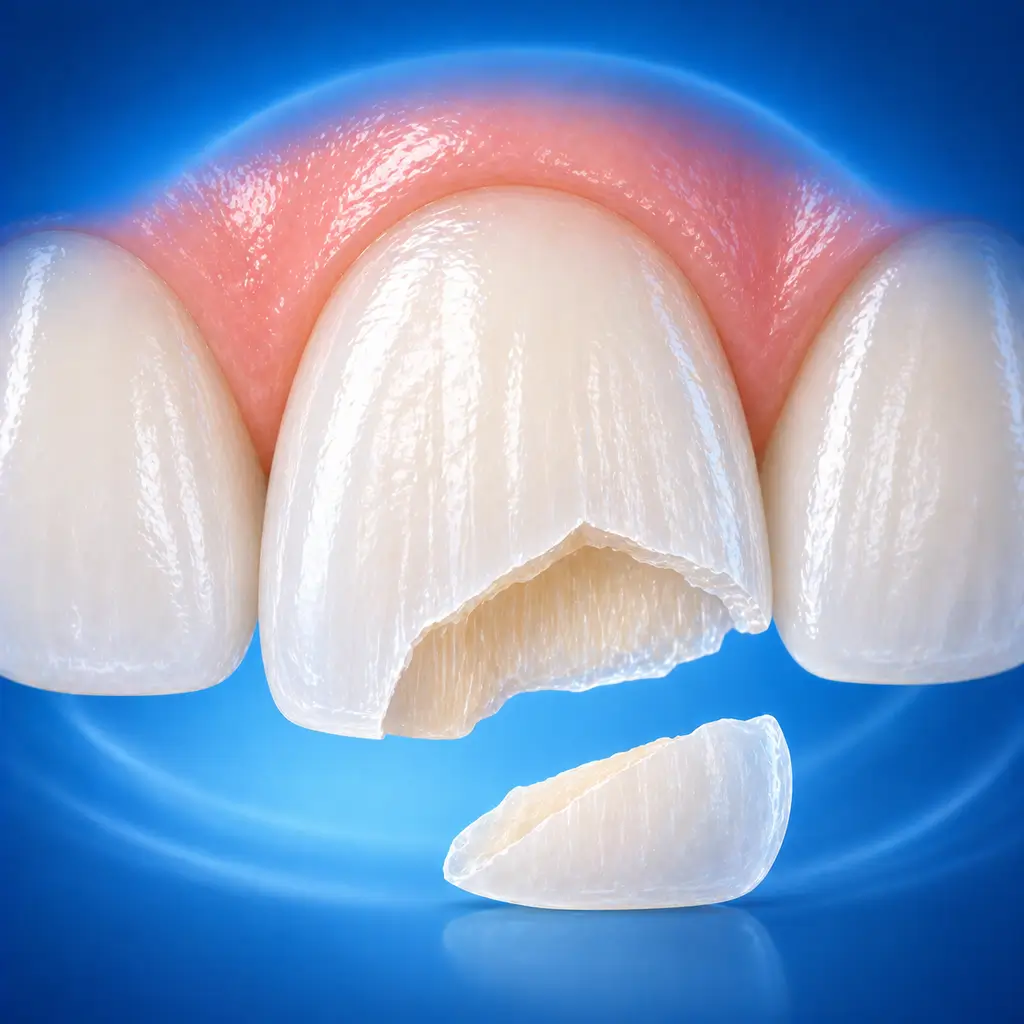
Common Symptoms
Recognizing Tooth fracture
Focus on the most useful decision cues first: common symptoms, the patients or situations that usually prompt review, and any signs that need faster assessment.
Common Symptoms
Signs patients often notice before evaluation
Visible loss of part of the crown, cracks, or tooth structure collapse
Root fracture may have an intact-looking crown but mobility or discoloration
Biting pain, percussion pain, cold/heat sensitivity or pain, spontaneous pain, or night pain
Root fracture or crown-root fracture may cause abnormal tooth mobility, sometimes with displacement
When crown-root fracture or root fracture extends below the gingiva, local gingival bleeding, redness, or swelling may occur
After pulp necrosis, the crown gradually turns gray or dark
When to Seek Evaluation
Typical patients and situations that warrant review
Common in children and adolescents
Visible tooth defect, crack, or fracture after external force
Biting pain, percussion pain, tooth mobility, or displacement after trauma
Severe pain from cold/heat stimulation, spontaneous pain, or night pain
Urgent Assessment
After a tooth fracture, seek immediate care if pulp exposure, persistent severe pain, obvious tooth mobility or displacement, gingival laceration with uncontrolled bleeding, or associated maxillofacial swelling, bite change, dizziness, vomiting, or other trauma signs occur.
Treatment Approaches
Treatment Directions for Tooth fracture
If only enamel is involved and there is no sensitivity, sharp edges may be smoothed and the fragment bonded or resin restoration placed
When dentin is exposed, dentin should be sealed promptly, with pulp protection when necessary, and tooth shape restored
For pulp exposure, direct pulp capping, pulpotomy, or root canal treatment is selected according to age, exposure time, contamination degree, and root development stage
Crown-root fracture or root fracture requires decisions about reduction and splinting, crown lengthening, orthodontic extrusion, root canal treatment, or extraction based on fracture position, mobility, periodontal support, and root length
In children and immature permanent teeth, vital pulp preservation and continued root development should be prioritized when possible, with regular postoperative follow-up of pulp and periapical status
What usually shapes the treatment plan
Clinical Assessment
Key Assessments for Tooth fracture
These are the main areas doctors usually review first. If you already have relevant test or imaging reports, bring them to speed up the assessment. They are helpful but not required, and the same workup can also be completed in China.
Fracture site and extent
Whether pulp exposure is present and pulp status
Whether tooth mobility is present
Displacement or luxation
Whether alveolar bone fracture or soft tissue laceration is present
Patient age and degree of root development
Determine whether the affected tooth can be retained
Before You Travel
How to Prepare
If the broken tooth fragment is found, place it in saline, milk, or a clean container and bring it to the hospital
Avoid biting hard objects with the affected tooth; if bleeding occurs, gently press with clean gauze
If trauma is accompanied by dizziness, vomiting, abnormal consciousness, obvious bite changes, or concern for facial fracture, go first to a general hospital emergency department
Planning Notes
Pre-Assessment Required
An oral specialist should perform an intraoral examination and, as appropriate, periodontal probing, pulp vitality testing, periapical radiographs, panoramic radiographs, or CBCT before determining the treatment plan. Key checks include visual assessment of defect extent, pulp exposure, tooth displacement, and gingival laceration; percussion to assess periapical or root-fracture response; palpation and mobility testing recorded in millimeters; and occlusal examination for premature contact or interference. Bring imaging and specialist oral examination records if available.
Remote Pre-Assessment
Intraoral photos, the course of pain/swelling, previous dental records, and imaging can be submitted remotely for preliminary triage, urgency assessment, and an estimated treatment direction. Final diagnosis still requires in-person intraoral examination and necessary imaging.
Multidisciplinary Assessment
Medical History Important
Previous dental treatment history, imaging, allergy history, anticoagulant/bisphosphonate use, diabetes, and immune-related diseases can affect diagnosis, anesthesia, bleeding and infection risk, and treatment selection.
Ready to Explore Treatment for Tooth fracture?
Let Carevia help you connect with the right specialists, compare hospitals, and plan your medical trip to China.