Wisdom tooth pericoronitis
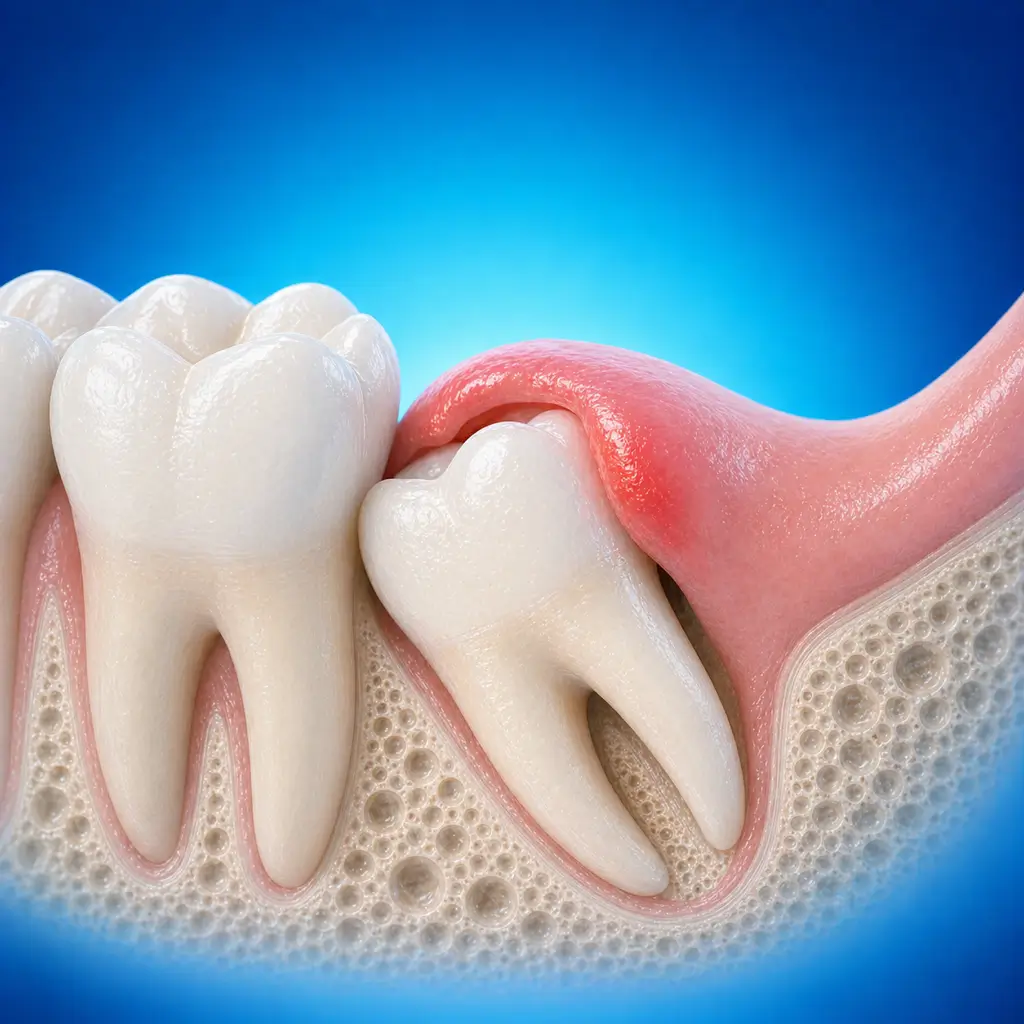
Infection of the soft tissue pocket around a partially erupted or impacted wisdom tooth. Acute episodes can cause pain and swelling, and severe cases require prevention of spread to maxillofacial fascial spaces.
Common Symptoms
Recognizing Wisdom tooth pericoronitis
Focus on the most useful decision cues first: common symptoms, the patients or situations that usually prompt review, and any signs that need faster assessment.
Common Symptoms
Signs patients often notice before evaluation
Swelling and pain in the retromolar area on the affected side, worse with chewing, swallowing, or mouth opening
May progress to spontaneous throbbing pain radiating to the ear and temporal area
Limited mouth opening; severe cases may cause trismus
Systemic symptoms: fever, headache, and fatigue
When to Seek Evaluation
Typical patients and situations that warrant review
Young adults aged 18-30 during wisdom tooth eruption, especially ages 20-29
No significant sex difference
Higher risk in pregnant women, menstruating women, and people with diabetes
Persistent redness, swelling, and pain around a wisdom tooth
Pain affecting eating, swallowing, or mouth opening
Spontaneous throbbing pain
Pus-like discharge visible from the pocket
Urgent Assessment
If facial or floor-of-mouth swelling expands rapidly, mouth opening is markedly limited, fever or chills occur, swallowing is difficult, breathing is impaired, or severe fatigue develops, seek immediate evaluation in oral and maxillofacial surgery or emergency care to prevent spread into fascial spaces.
Treatment Approaches
Treatment Directions for Wisdom tooth pericoronitis
During the acute phase, local irrigation, medication, and systemic anti-infective treatment are the main approaches
If an abscess has formed, incision and drainage are performed
After inflammation subsides, gingival flap excision or wisdom tooth extraction is performed depending on the situation
What usually shapes the treatment plan
Clinical Assessment
Key Assessments for Wisdom tooth pericoronitis
These are the main areas doctors usually review first. If you already have relevant test or imaging reports, bring them to speed up the assessment. They are helpful but not required, and the same workup can also be completed in China.
Severity of inflammation
Whether an abscess has formed
Type of wisdom tooth impaction
Degree of limited mouth opening
Signs of systemic infection
Frequency of previous episodes
Before You Travel
How to Prepare
If available, prepare previous oral imaging and systemic medical records
Planning Notes
Pre-Assessment Required
An oral specialist should perform an intraoral examination and, as appropriate, periodontal probing, pulp vitality testing, periapical radiographs, panoramic radiographs, or CBCT before determining the treatment plan. Key checks include specialist oral examination; complete blood count to assess infection severity; dental radiographs or panoramic imaging to assess wisdom tooth position, impaction type, and relationship to the mandibular nerve canal; and bacterial culture plus susceptibility testing in severe cases. Also bring previous panoramic radiographs, CBCT, and blood count results if available.
Remote Pre-Assessment
Intraoral photos, the course of pain/swelling, previous dental records, and imaging can be submitted remotely for preliminary triage, urgency assessment, and an estimated treatment direction. Final diagnosis still requires in-person intraoral examination and necessary imaging.
Multidisciplinary Assessment
Medical History Important
Previous dental treatment history, imaging, allergy history, anticoagulant/bisphosphonate use, diabetes, and immune-related diseases can affect diagnosis, anesthesia, bleeding and infection risk, and treatment selection.
Ready to Explore Treatment for Wisdom tooth pericoronitis?
Let Carevia help you connect with the right specialists, compare hospitals, and plan your medical trip to China.