Cracked tooth
Fine cracks in a tooth can cause biting pain or cold/heat sensitivity. Early assessment of crack depth and tooth protection are needed to prevent progression to pulpitis or tooth fracture.
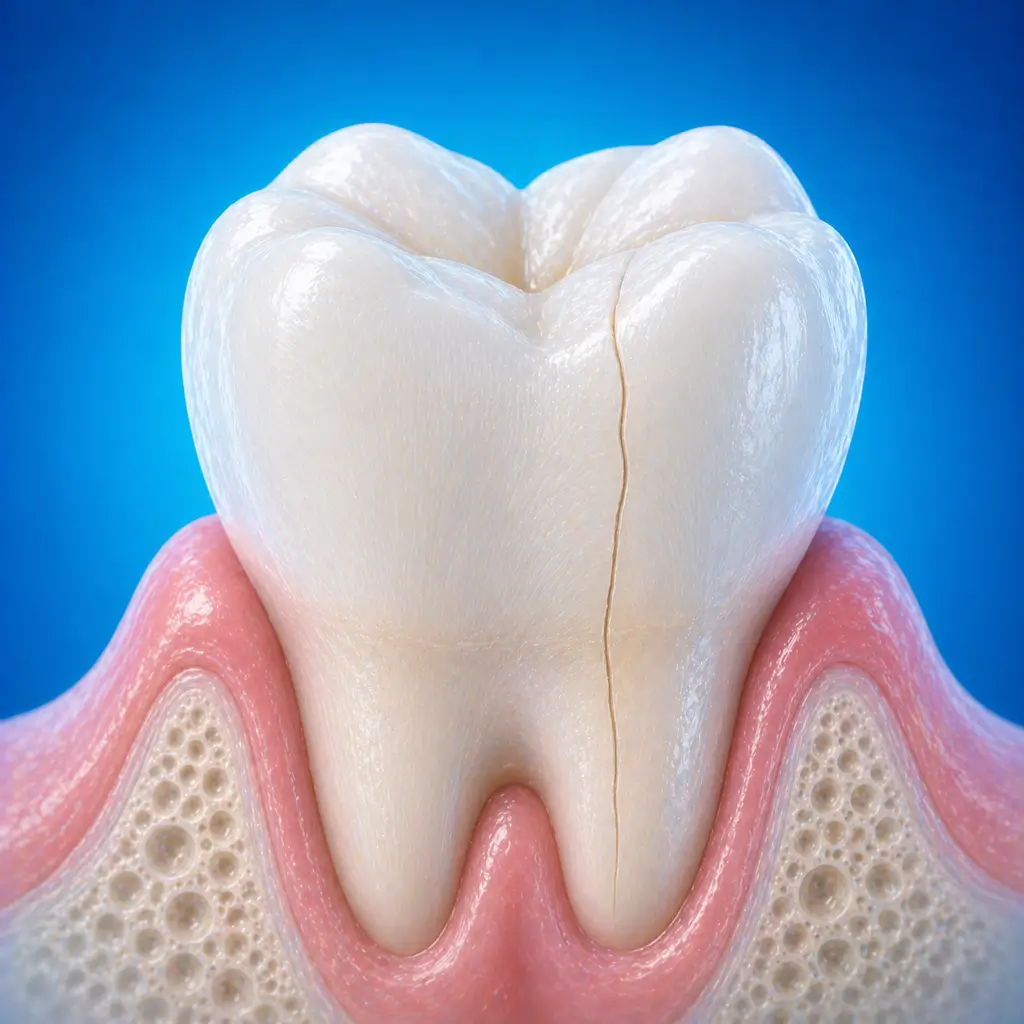
Common Symptoms
Recognizing Cracked tooth
Focus on the most useful decision cues first: common symptoms, the patients or situations that usually prompt review, and any signs that need faster assessment.
Common Symptoms
Signs patients often notice before evaluation
Severe pain at a specific biting point: when food or a cusp acts exactly on the crack during chewing, an instantaneous sharp stabbing pain occurs and disappears immediately after release. This is the most typical feature of a cracked tooth
Cold and heat sensitivity: when the crack reaches dentin, transient sensitivity occurs with cold or heat stimuli
If the crack reaches the pulp, persistent pulpitis-like pain may occur
Spontaneous pain or night pain occurs when the crack has involved the pulp and caused irreversible pulpitis
Tooth sensitivity: soreness after chewing or drinking cold beverages, with difficulty locating the affected tooth
Split tooth: when the crack extends completely to the root or the tooth structure collapses, partial or complete tooth fracture may occur
When to Seek Evaluation
Typical patients and situations that warrant review
Common in middle-aged and older adults, more often in men
Transient sharp pain when chewing hard food or biting in a specific position, without obvious caries
Pain triggered by cold or heat that disappears immediately or lasts several seconds after the stimulus is removed
Pulpitis-like symptoms without an obvious cause, such as spontaneous pain or night pain
Unexplained biting discomfort or percussion pain
Treatment Approaches
Treatment Directions for Cracked tooth
Asymptomatic superficial cracks limited to enamel may be observed regularly or treated with sealant/preventive resin filling
Cracks reaching dentin but not involving the pulp and without pulpitis symptoms may be protected with a full crown to prevent crack progression
For reversible pulpitis, sedative treatment or direct pulp capping may be performed first, followed by full crown restoration after symptoms resolve
For irreversible pulpitis, root canal treatment is needed first, followed immediately by full crown restoration because root canal treated teeth are more prone to splitting
If the crack has extended to the root surface or furcation, causing a periodontal pocket or pulpal floor perforation, the tooth usually cannot be retained and extraction is needed
What usually shapes the treatment plan
Clinical Assessment
Key Assessments for Cracked tooth
These are the main areas doctors usually review first. If you already have relevant test or imaging reports, bring them to speed up the assessment. They are helpful but not required, and the same workup can also be completed in China.
Crack depth, including whether it reaches the pulp or extends to the root surface
Identify the source of biting pain, excluding reversible pulpitis, periodontal disease, and periapical periodontitis
Assess pulp status, normal, reversible, irreversible, or necrotic
Determine whether the affected tooth can be retained
Before You Travel
How to Prepare
Bring imaging records and previous dental treatment history
Planning Notes
Pre-Assessment Required
An oral specialist should perform an intraoral examination and, as appropriate, periodontal probing, pulp vitality testing, periapical radiographs, panoramic radiographs, or CBCT before determining the treatment plan. Key checks include visual examination with oblique strong light to identify suspicious cracks, sometimes seen as thin dark lines; probing along fissures or cracks with a sharp explorer, which may catch in the crack or trigger pain; percussion, where pain in a specific direction may be positive; and bite testing with a rubber wheel, cotton roll, or special bite tool such as a Fraxfinder to reproduce the typical instant sharp pain. A common method is having the patient bite on a cotton roll or dental instrument handle from different angles and release to see whether pain is reproduced. Bring specialist oral examination and imaging records if available.
Remote Pre-Assessment
Intraoral photos, the course of pain/swelling, previous dental records, and imaging can be submitted remotely for preliminary triage, urgency assessment, and an estimated treatment direction. Final diagnosis still requires in-person intraoral examination and necessary imaging.
Multidisciplinary Assessment
Medical History Important
Previous dental treatment history, imaging, allergy history, anticoagulant/bisphosphonate use, diabetes, and immune-related diseases can affect diagnosis, anesthesia, bleeding and infection risk, and treatment selection.
Ready to Explore Treatment for Cracked tooth?
Let Carevia help you connect with the right specialists, compare hospitals, and plan your medical trip to China.