Intravitreal Anti-VEGF Injection
Anti-vascular endothelial growth factor (VEGF) medication is precisely injected into the vitreous cavity to suppress pathological neovascularization and vascular leakage — the first-line treatment for wet AMD, diabetic macular edema, and retinal vein occlusion macular edema.
Intravitreal anti-VEGF injection is the gold-standard treatment for macular edema and choroidal neovascularization (CNV) caused by a range of retinal vascular diseases. VEGF is the key driver of pathological neovascularization and vascular hyperpermeability; anti-VEGF agents specifically bind VEGF, blocking its receptor interaction and thereby inhibiting new vessel growth, reducing vascular leakage and macular edema, and preserving or improving central vision. Currently approved agents include ranibizumab (Novartis; Lucentis), aflibercept (Bayer; Eylea; domestic biosimilars now available), bevacizumab (off-label), and conbercept (Chengdu Kanghong; Langmu — a Chinese-developed agent with a multi-VEGF-family binding profile). Drug choice depends on disease type, severity, required injection interval, and cost considerations. Intravitreal injection is an outpatient procedure performed under topical anesthesia with strict asepsis. A fine needle is inserted 3.5-4 mm posterior to the limbus (pars plana) and 0.05 mL of drug is delivered into the vitreous cavity. The procedure takes approximately 5 minutes; post-injection observation of 30-60 minutes confirms there is no acute IOP elevation before discharge.
Quick Reference
Treatment
5 mins – 15 mins
Observation
30 mins – 1 hours
Est. Cost
¥877.88 – ¥2,633.63
Department
Ophthalmology
Who Is This For
Is Intravitreal Anti-VEGF Injection Right for You?
Good Candidates
- Neovascular (wet) age-related macular degeneration (nAMD) with active CNV
- Diabetic macular edema (DME) involving or threatening the center of the macula
- Macular edema secondary to central or branch retinal vein occlusion (CRVO/BRVO)
- Myopic CNV (pathologic myopia-associated choroidal neovascularization)
- Other anti-VEGF indications (e.g., retinopathy of prematurity)
May Not Be Suitable
- Active periocular or intraocular infection (injection must be deferred until infection is controlled)
- Known hypersensitivity to the specific anti-VEGF agent or its components
- Very low baseline IOP (hypotony may be worsened by injection)
- Severe coagulation disorder (relative contraindication — risk-benefit must be assessed)
- End-stage retinal disease with minimal residual visual function where meaningful benefit is unlikely
Step-by-Step Process
How Intravitreal Anti-VEGF Injection Works
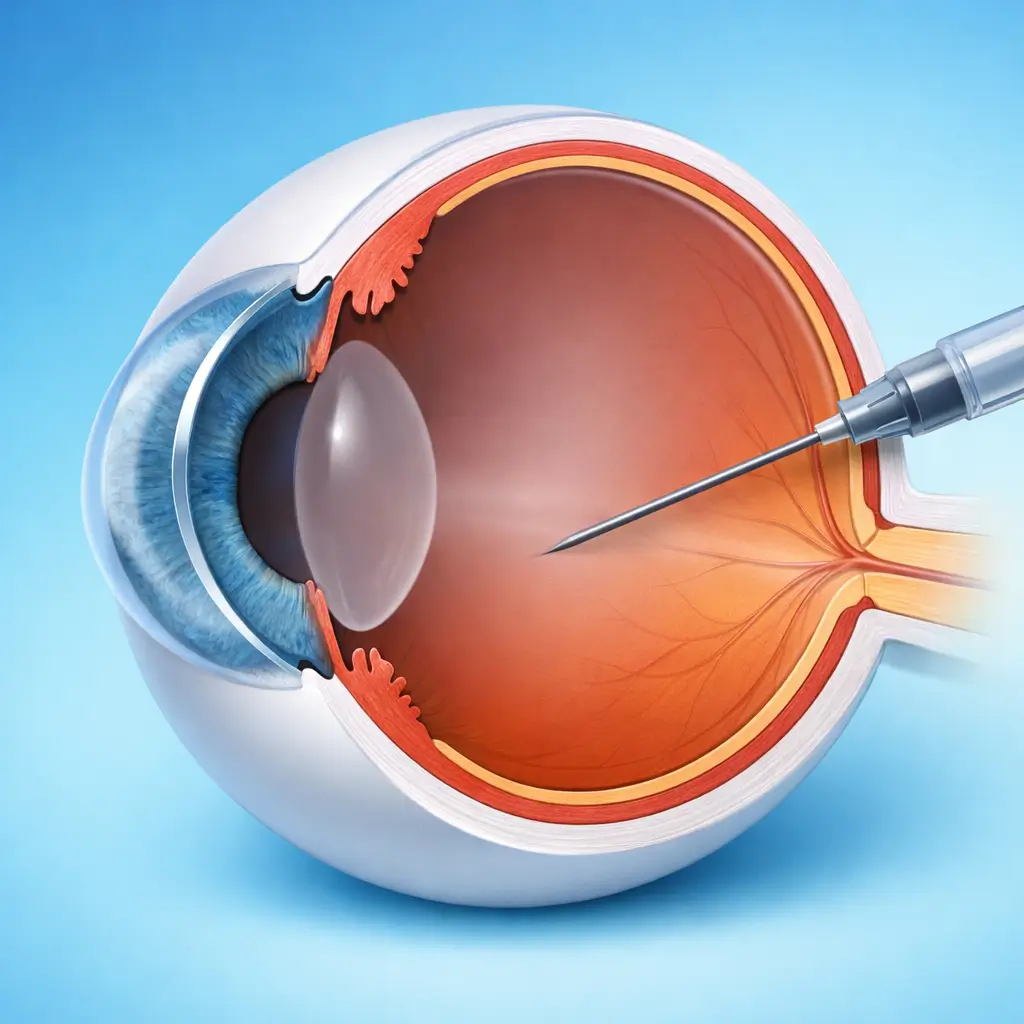
Preparation and Antisepsis
The patient lies supine. Topical anesthetic drops are instilled. The ocular surface is sterilized with 5% povidone-iodine (conjunctival sac irrigation + periocular skin preparation). Strict aseptic technique is maintained throughout to prevent infectious endophthalmitis. A lid speculum is placed.
Injection Site Marking
A caliper marks the injection site 3.5-4 mm posterior to the limbus in the inferotemporal quadrant (the preferred avascular zone). The planned needle trajectory is confirmed to be clear of the crystalline lens.
Intravitreal Drug Delivery
A 30-gauge needle is inserted perpendicular to the sclera at the marked site and advanced into the vitreous cavity. 0.05 mL (50 μL) of anti-VEGF drug is slowly injected over approximately 5-10 seconds. The needle is withdrawn and the puncture site gently compressed with a cotton tip.
Immediate Post-Injection Assessment
The optic disc is promptly visualized by indirect ophthalmoscopy or slit lamp to assess for pallor indicating acute ischemia from IOP spike. IOP is measured and confirmed within an acceptable range.
Observation and Discharge
The patient waits in the clinic for 30-60 minutes. A second IOP check and symptom inquiry are performed before discharge. Written aftercare instructions are provided, clearly describing the symptoms of endophthalmitis and emergency contact procedures.
Anti-VEGF injection is a long-term, chronic disease management strategy requiring repeated treatment. Common protocols include an initial loading phase (3 monthly injections), followed by a pro re nata (PRN) or treat-and-extend (T&E) maintenance phase with injection intervals adjusted based on OCT findings. Wet AMD patients average 4-8 injections per year; DME patients average 5-8, depending on disease stability.
Cost Information
Cost Estimate for Intravitreal Anti-VEGF Injection
Estimated Price Range
¥877.88 – ¥2,633.63
What's Included
Public tier-3A International Medical Department: imported drug (ranibizumab/aflibercept) approximately ¥6,000-10,000 per eye per injection; domestic conbercept approximately ¥4,500-7,000 per eye. Premium private eye centers: imported drug approximately ¥10,000-18,000 per injection, including comprehensive preoperative OCT assessment and follow-up management. Cost variation mainly stems from drug choice and service package.
Before Your Visit
What to Prepare
Required Tests & Examinations
If you already have recent valid test results, bring the reports. If not, these assessments can usually be completed in China before the procedure.
Macular OCT (structural assessment of retinal edema and CNV activity — the key monitoring tool)
Fundus fluorescein angiography (FFA) and/or indocyanine green angiography (ICGA — characterize CNV type and extent)
Best corrected visual acuity (BCVA — document baseline)
Color fundus photography (document lesion extent)
Intraocular pressure measurement
Systemic blood pressure and blood glucose (essential for diabetic patients)
Documents & Materials to Bring
Required to Bring
Recent macular OCT and fundus angiography reports
Systemic disease records (diabetes, hypertension, coagulation disorders)
Current medication list (especially anticoagulants)
Prior anti-VEGF injection history (drug name, number of injections, treatment response)
Passport and valid visa
Companion & Support
A companion is required on the injection day, as transient visual disturbance and occasional procedural anxiety may prevent the patient from traveling independently. For patients on frequent injection schedules, it is important that family members recognize the symptoms of endophthalmitis and know the emergency contact process.
After Treatment
Recovery & Follow-Up
Subconjunctival hemorrhage (red eye patch) is common, harmless, and resolves spontaneously within 1-2 weeks; mild foreign-body sensation and increased floaters from the medication bubble are also normal
Avoid water contact with the eye and do not rub the eye for 24 hours after injection
Seek emergency care immediately if eye pain worsens significantly, vision drops sharply, or discharge increases in the 3 days post-injection — these may signal infectious endophthalmitis (most serious complication; incidence ~1/3,000; outcomes are best with prompt treatment)
Tight systemic risk factor control (blood glucose, blood pressure) is critical to slowing disease progression
Adhere strictly to the follow-up schedule — do not self-discontinue treatment because vision appears temporarily stable
Follow-Up Schedule
OCT review is usually performed 4-8 weeks after each injection to assess macular edema resolution and CNV activity, determining whether the next injection is indicated. Most diseases require long-term follow-up, but the frequency and total treatment duration depend on diagnosis, lesion activity, and treatment response.
Related Conditions
Conditions This Procedure Treats
Ready to Plan Intravitreal Anti-VEGF Injection in China?
Let Carevia help you find the right hospital, coordinate your treatment, and arrange every detail of your medical trip.
Frequently Asked Questions
Need personalized guidance?
Our care coordinators can help you assess whether this procedure fits your situation.
Contact Us