Periodontitis
Chronic inflammatory destruction of the tooth-supporting tissues, often presenting with gum bleeding, periodontal pockets, and tooth mobility. It is an important cause of tooth loss in adults.
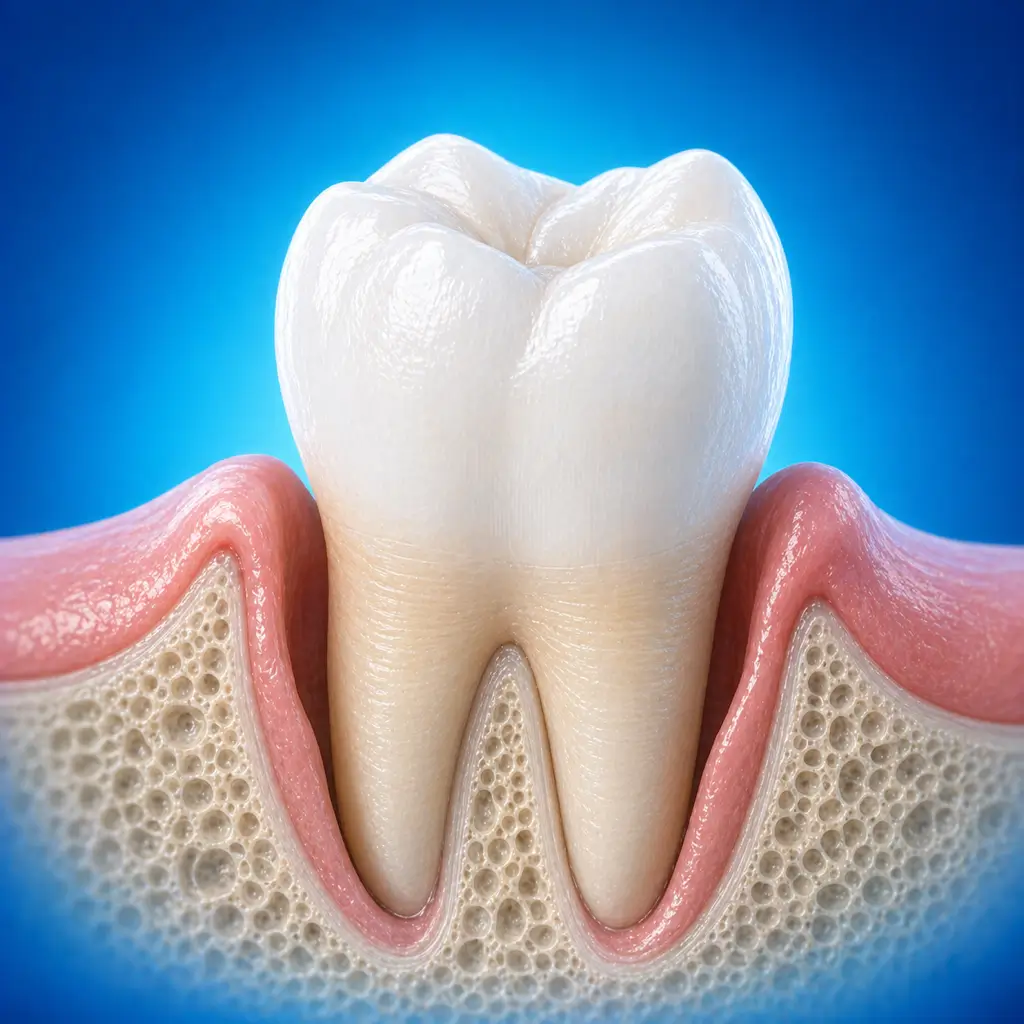
Common Symptoms
Recognizing Periodontitis
Focus on the most useful decision cues first: common symptoms, the patients or situations that usually prompt review, and any signs that need faster assessment.
Common Symptoms
Signs patients often notice before evaluation
Red, swollen, bleeding gums; gingival recession; periodontal pocket formation; tooth mobility or migration; weak or uncomfortable biting; bad breath
Periodontal abscess: during acute episodes, poor drainage from the periodontal pocket can form localized gingival swelling, pain, and fluctuation, with lymph node enlargement and fever
Furcation involvement: bone destruction in the root furcation area of multi-rooted teeth, where a probe can enter
When to Seek Evaluation
Typical patients and situations that warrant review
Common in adults, especially middle-aged and older adults. Aggressive periodontitis is more common in adolescents and young adults
Red, swollen, bleeding gums; gingival recession; periodontal pocket formation; tooth mobility or migration; weak or uncomfortable biting; bad breath
Treatment Approaches
Treatment Directions for Periodontitis
Treatment principles are plaque control, elimination of inflammation, stabilization of periodontal support, and establishment of long-term maintenance
Basic treatment includes oral hygiene instruction, supragingival scaling, subgingival scaling and root planing, and management of defective restorations, food impaction, and occlusal trauma when needed
After basic treatment, periodontal pocket depth, bleeding on probing, and plaque control are usually rechecked. If deep pockets or complex bone defects remain, periodontal surgery may be considered
Teeth with severe mobility, repeated acute abscesses, or poor retention value require extraction assessment
Smokers should quit or reduce smoking, and patients with diabetes should control blood glucose at the same time. After stabilization, periodontal maintenance is performed every 3-6 months
What usually shapes the treatment plan
Clinical Assessment
Key Assessments for Periodontitis
These are the main areas doctors usually review first. If you already have relevant test or imaging reports, bring them to speed up the assessment. They are helpful but not required, and the same workup can also be completed in China.
Periodontal pocket depth and clinical attachment loss
Type and extent of alveolar bone resorption
Tooth mobility and migration
Presence and grade of furcation involvement
Whether periodontal abscess is present
Whether occlusal trauma is present
Amount and distribution of plaque and calculus
Systemic risk factors, such as smoking, diabetes, and genetics
Patient adherence
Before You Travel
How to Prepare
Bring imaging records and recent blood test reports if available
Planning Notes
Pre-Assessment Required
A full-mouth periodontal examination is needed, recording probing depth at six sites per tooth, clinical attachment loss, bleeding on probing, suppuration, mobility, and furcation involvement, combined with periapical radiographs, panoramic radiographs, or CBCT to assess alveolar bone loss. Diabetes, smoking, pregnancy, immune status, and medication history affect treatment planning and follow-up frequency.
Remote Pre-Assessment
Intraoral photos, the course of pain/swelling, previous dental records, and imaging can be submitted remotely for preliminary triage, urgency assessment, and an estimated treatment direction. Final diagnosis still requires in-person intraoral examination and necessary imaging.
Multidisciplinary Assessment
Medical History Important
Previous dental treatment history, imaging, allergy history, anticoagulant/bisphosphonate use, diabetes, and immune-related diseases can affect diagnosis, anesthesia, bleeding and infection risk, and treatment selection.
Ready to Explore Treatment for Periodontitis?
Let Carevia help you connect with the right specialists, compare hospitals, and plan your medical trip to China.