Keratoconus
A progressive corneal thinning and cone-shaped protrusion disorder causing irregular astigmatism and vision loss.
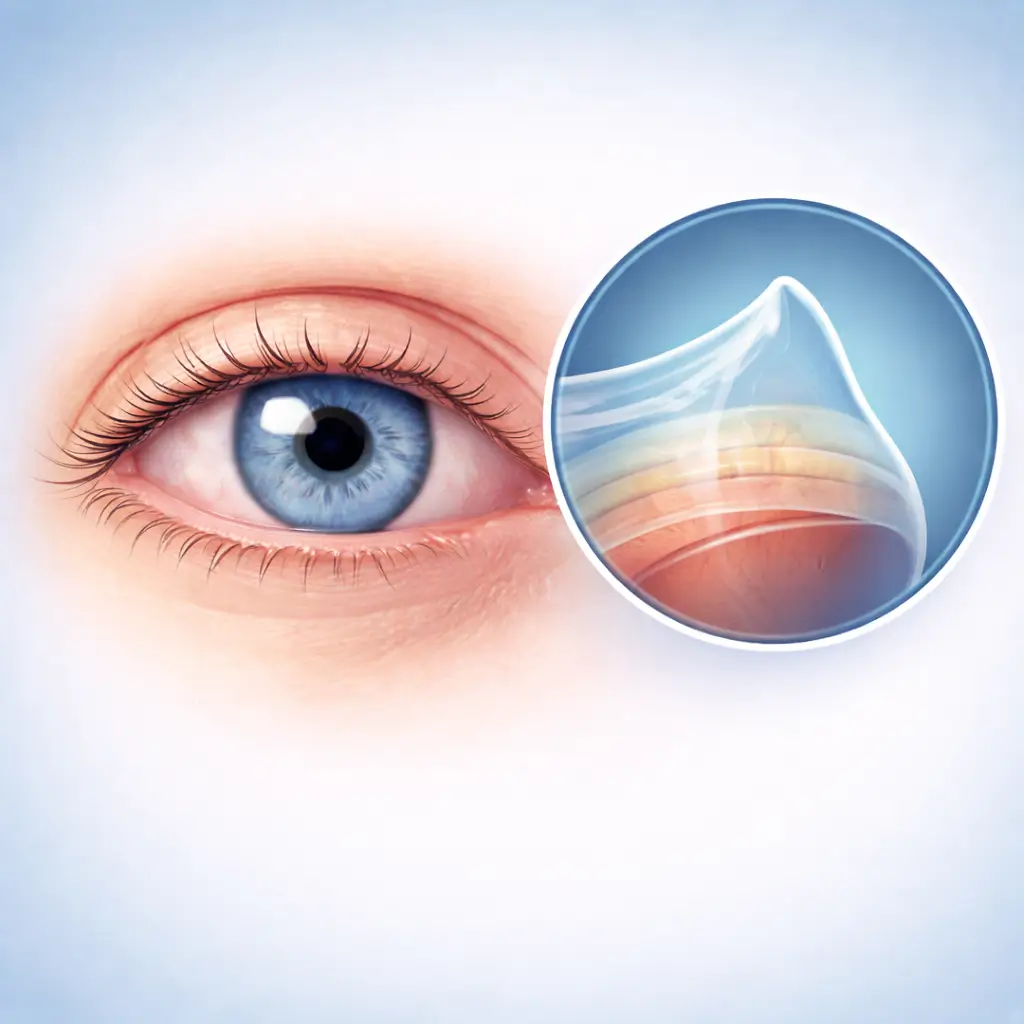
Common Symptoms
Recognizing Keratoconus
Focus on the most useful decision cues first: common symptoms, the patients or situations that usually prompt review, and any signs that need faster assessment.
Common Symptoms
Signs patients often notice before evaluation
Progressive vision loss with decreasing spectacle correction effectiveness
Frequent changes in glasses prescription
Steadily increasing astigmatism
Poor night vision with significant halos
Corneal edema in severe thinning (acute hydrops)
When to Seek Evaluation
Typical patients and situations that warrant review
Adolescents and young adults (typically onset at 10-25 years)
Those who frequently rub their eyes
Allergic conjunctivitis patients
Those with family history of keratoconus
Down syndrome patients
Increasing astigmatism with poor spectacle correction
Suspected corneal ectasia found during refractive surgery screening
Confirmed keratoconus requiring progression and treatment assessment
Treatment Approaches
Treatment Directions for Keratoconus
Corneal cross-linking CXL (early stage to halt progression)
Rigid gas permeable RGP/scleral contact lenses (correct irregular astigmatism)
ICL implantation (address the refractive error component)
Corneal transplantation (advanced severe cases)
What usually shapes the treatment plan
Clinical Assessment
Key Assessments for Keratoconus
These are the main areas doctors usually review first. If you already have relevant test or imaging reports, bring them to speed up the assessment. They are helpful but not required, and the same workup can also be completed in China.
Corneal topography (Pentacam, critical for diagnosis and progression assessment)
Corneal thickness mapping (thinnest point localization)
Slit-lamp examination (Vogt striae, Fleischer ring)
Corneal biomechanical testing
Refraction and best corrected visual acuity
Before You Travel
How to Prepare
Discontinue contact lenses (soft lenses at least 1 week, RGP at least 2 weeks)
Bring previous corneal topography maps for progression comparison
Stop eye rubbing
Planning Notes
Pre-Assessment Required
Pentacam corneal topography, pachymetry maps, and corneal biomechanical testing are needed to assess keratoconus staging, progression risk, and optimal treatment plan.
Remote Pre-Assessment
Corneal topography maps and previous examination reports can be submitted remotely for preliminary staging and progression assessment. Specific surgical evaluation requires on-site examination.
Multidisciplinary Assessment
Medical History Important
Allergy history and eye rubbing habits are important; serial corneal topography changes are crucial for assessing progression rate.
Ready to Explore Treatment for Keratoconus?
Let Carevia help you connect with the right specialists, compare hospitals, and plan your medical trip to China.