Retinal Laser Photocoagulation
Laser energy destroys ischemic retinal tissue to reduce VEGF secretion, halt pathological neovascularization, and prevent sight-threatening complications — a cornerstone treatment for diabetic retinopathy and retinal vein occlusion.
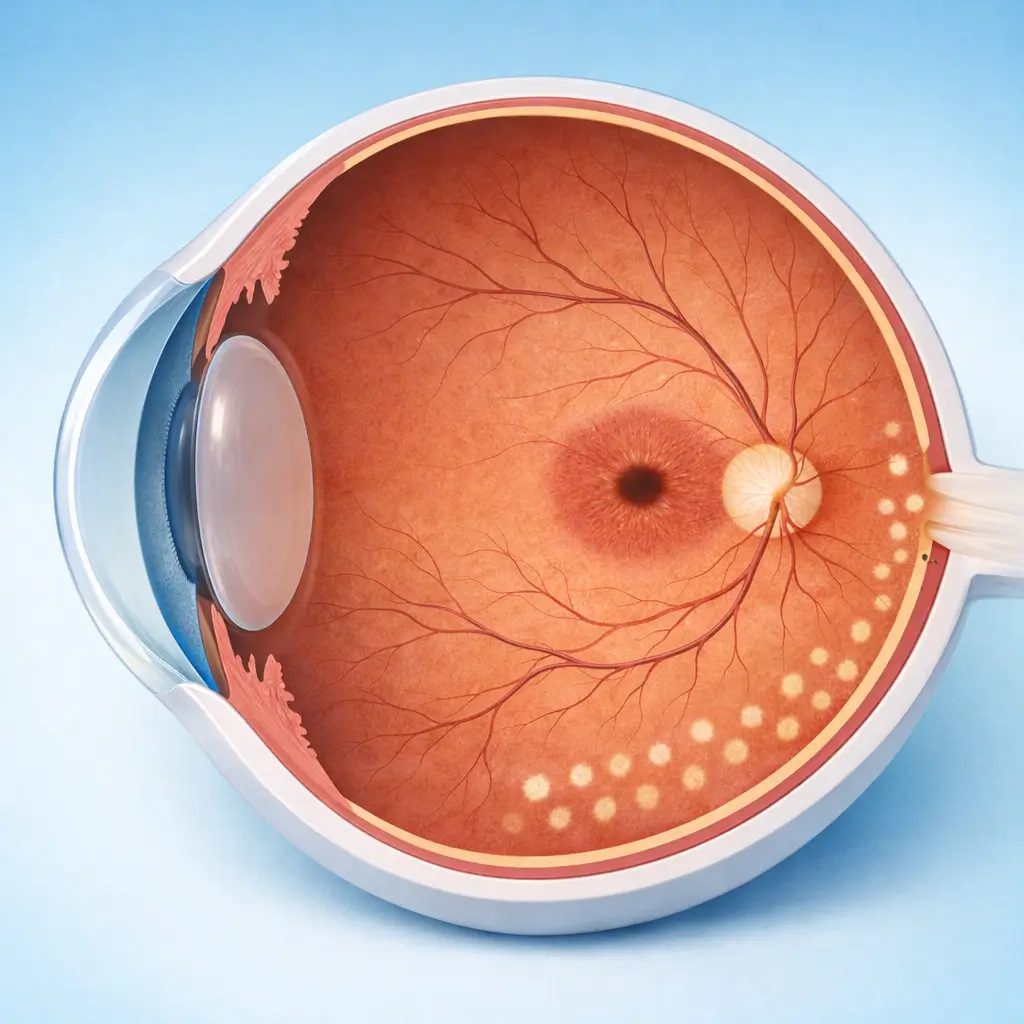
Retinal laser photocoagulation has been a mainstay of retinal vascular disease treatment for over 60 years and remains a standard of care for diabetic retinopathy (DR) and retinal vein occlusion (RVO). Laser energy absorbed by the retinal pigment epithelium creates focal thermal coagulation, destroying ischemic photoreceptors in areas of poor perfusion. By reducing the metabolic oxygen demand of these zones, total retinal VEGF production decreases, inhibiting pathological neovascularization and preventing serious complications such as vitreous hemorrhage and tractional retinal detachment. There are three main modalities: Pan-retinal photocoagulation (PRP) — used for proliferative DR (PDR) or extensive ischemic RVO, delivering 1,500-2,000 laser spots across the peripheral retina (sparing the macula and disc), typically over 2-3 sessions; Focal photocoagulation — direct treatment of leaking microaneurysms in non-center-involving diabetic macular edema; Grid photocoagulation — a grid pattern of burns over edematous retina (largely superseded by anti-VEGF injection for macular edema). While anti-VEGF injections have replaced laser as the primary treatment for macular edema, PRP remains irreplaceable for managing new vessels in PDR and preventing catastrophic complications. Its lower cost and avoidance of repeated injections make it a critical option in resource-limited settings and a complementary tool in comprehensive retinal care.
Quick Reference
Treatment
15 mins – 45 mins
Observation
30 mins – 1 hours
Est. Cost
¥512.1 – ¥2,048.38
Department
Ophthalmology
Who Is This For
Is Retinal Laser Photocoagulation Right for You?
Good Candidates
- Proliferative diabetic retinopathy (PDR) with neovascularization requiring PRP
- Severe non-proliferative DR (NPDR) with high-risk features — preventive PRP
- Ischemic central or branch retinal vein occlusion with extensive non-perfusion
- Non-center-involving diabetic macular edema with focal leaking microaneurysms (focal laser)
- Retinal breaks or lattice degeneration — prophylactic retinopexy to prevent retinal detachment
May Not Be Suitable
- Dense vitreous hemorrhage obscuring the retina (vitrectomy needed first to clear media)
- Significant corneal or lens opacity preventing adequate laser transmission to the retina
- Center-involving diabetic macular edema (anti-VEGF injection is preferred; laser risks foveal damage)
- Established retinal detachment (detached retina does not respond to laser; surgical reattachment is required)
- Patients unable to cooperate with fixation during treatment
Step-by-Step Process
How Retinal Laser Photocoagulation Works
Dilation and Anesthesia
Full mydriasis is achieved (compound tropicamide; ~30 minutes). Topical anesthetic drops are instilled. Peribulbar anesthesia may be added for PRP to reduce the significant discomfort from high spot counts.
Contact Lens Placement
A laser contact lens (e.g., Mainster wide-field or Volk QuadrAspheric) coupled with methylcellulose is placed on the cornea to obtain a clear fundus image and focus the laser beam.
Laser Parameter Selection
532 nm green or 577 nm yellow laser is commonly used. Parameters: spot size 200-500 μm, exposure duration 0.1-0.2 seconds, power titrated to produce a mild grey-white reaction (Grade II burn) without excessive coagulation.
Laser Application
The physician delivers laser spots sequentially across the target area through the slit-lamp delivery system. PRP spots are distributed uniformly from the posterior pole margin to the periphery, strictly avoiding the fovea and optic disc. Focal laser precisely targets leaking microaneurysms. Each session lasts 15-45 minutes.
Post-Treatment Assessment and Discharge
The contact lens is removed and the ocular surface rinsed. IOP is checked (transient elevation is occasionally seen). Vision is blurred due to mydriasis — patients wait 30-60 minutes for partial pupil recovery before departing.
PRP is typically divided into 2-3 sessions (1-2 weeks apart) to avoid precipitating a macular edema flare from a large single-session spot count. Focal/grid laser may be completed in a single session with repeat treatment at 3 months if FFA shows persistent leakage.
Cost Information
Cost Estimate for Retinal Laser Photocoagulation
Estimated Price Range
¥512.1 – ¥2,048.38
What's Included
Public tier-3A International Medical Department: focal/grid photocoagulation approximately ¥3,500-6,000 per session; panretinal photocoagulation (PRP) approximately ¥5,000-8,000 per session, complete course (2-3 sessions) approximately ¥10,000-18,000. Premium private eye centers: PRP approximately ¥8,000-14,000 per session, including comprehensive preoperative FFA and OCT assessment with customized laser parameters and follow-up management.
Before Your Visit
What to Prepare
Required Tests & Examinations
If you already have recent valid test results, bring the reports. If not, these assessments can usually be completed in China before the procedure.
Fundus fluorescein angiography (FFA): map non-perfusion zones, new vessels, and leakage sites
Macular OCT: quantify macular edema type and severity
Color fundus photography: document baseline lesion extent
Best corrected visual acuity
Intraocular pressure measurement
Blood glucose and HbA1c (systemic control assessment for diabetic patients)
Documents & Materials to Bring
Required to Bring
Recent FFA and OCT reports
Diabetes diagnosis and glycemic control records (HbA1c)
Current systemic medication list
Passport and valid visa
After Treatment
Recovery & Follow-Up
Vision is blurred and light-sensitive from dilation for several hours — do not drive on the day of treatment
Mild eye ache or pressure is common for 1-2 days after PRP; oral analgesics may be used if needed
Some peripheral visual field constriction is expected after PRP — this is a deliberate trade-off to protect central (macular) vision
Night vision may be mildly reduced after PRP — this is a known treatment effect
Strict blood glucose and blood pressure control is as important as laser treatment in slowing diabetic retinopathy progression
Follow-Up Schedule
FFA and OCT review 1-2 months after each laser session to assess new vessel regression and determine whether supplemental treatment is needed; stable patients followed every 3-6 months.
Related Conditions
Conditions This Procedure Treats
Ready to Plan Retinal Laser Photocoagulation in China?
Let Carevia help you find the right hospital, coordinate your treatment, and arrange every detail of your medical trip.
Frequently Asked Questions
Need personalized guidance?
Our care coordinators can help you assess whether this procedure fits your situation.
Contact Us