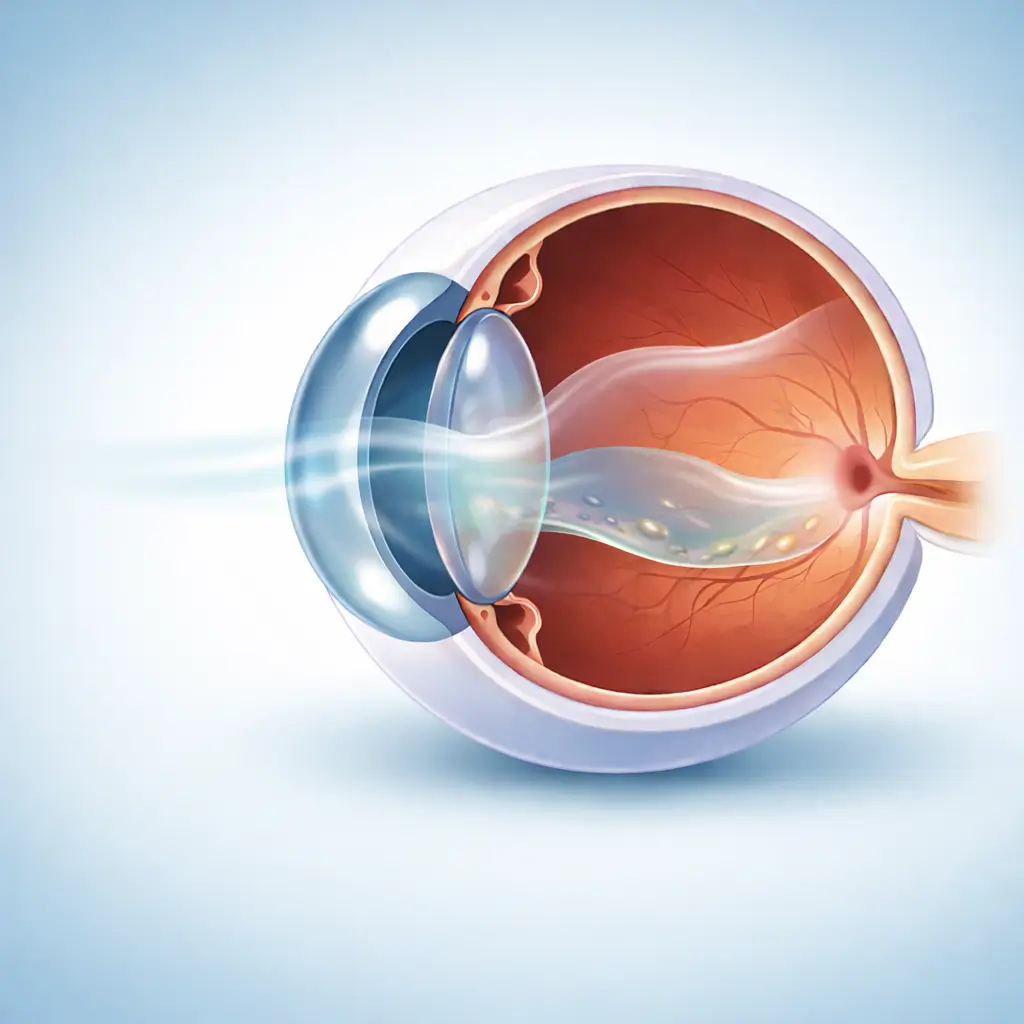
Retinal Detachment
An ophthalmic emergency where the retina separates from its underlying tissue, potentially causing permanent vision loss without timely surgery.
Common Symptoms
Recognizing Retinal Detachment
Focus on the most useful decision cues first: common symptoms, the patients or situations that usually prompt review, and any signs that need faster assessment.
Common Symptoms
Signs patients often notice before evaluation
Sudden onset of numerous floaters or flashes of light
Curtain-like shadow in visual field
Acute vision loss
Distorted vision
When to Seek Evaluation
Typical patients and situations that warrant review
High myopia patients (>-6.00D)
History of ocular trauma
Previous retinal detachment in the fellow eye
Previous intraocular surgery (e.g., post-cataract surgery)
Family history of retinal detachment
Sudden increase in floaters with flashes (possible retinal tear, seek care within 24 hours)
Curtain-like shadow in visual field (retina has detached, requires emergency care)
Urgent Assessment
Retinal detachment is an ophthalmic emergency! Seek immediate medical attention if you experience sudden increase in floaters, flashes of light, or curtain-like visual field obstruction. Surgery is most effective when the macula has not yet detached; delays may cause irreversible vision loss.
Treatment Approaches
Treatment Directions for Retinal Detachment
Pars plana vitrectomy (PPV, most commonly used surgical approach)
Scleral buckling (suitable for young patients with simple rhegmatogenous detachment and clear lens)
Gas or silicone oil tamponade (postoperative support for retinal reattachment)
Laser or cryotherapy to seal retinal breaks
What usually shapes the treatment plan
Clinical Assessment
Key Assessments for Retinal Detachment
These are the main areas doctors usually review first. If you already have relevant test or imaging reports, bring them to speed up the assessment. They are helpful but not required, and the same workup can also be completed in China.
Detailed dilated fundus examination
B-scan ultrasound (assess retinal status when vitreous is opaque)
OCT (evaluate macular involvement)
Visual field testing
Before You Travel
How to Prepare
Seek medical attention as soon as possible without delay
Maintain appropriate positioning (doctor may recommend specific head position to slow detachment)
Bring previous eye examination records
Planning Notes
Pre-Assessment Required
Urgent dilated fundus examination and B-scan ultrasound are needed to assess detachment extent, break location, and macular status, allowing rapid surgical planning.
Remote Pre-Assessment
Multidisciplinary Assessment
Medical History Important
High myopia degree, previous eye surgery history, and fellow eye status are important for surgical planning.
Ready to Explore Treatment for Retinal Detachment?
Let Carevia help you connect with the right specialists, compare hospitals, and plan your medical trip to China.