Maxillofacial space infection
Maxillofacial space infection is suppurative inflammation within potential fascial spaces of the maxillofacial region, most often caused by spread of odontogenic infection. Severe cases can be life-threatening and are among the most common serious emergencies in oral and maxillofacial surgery.
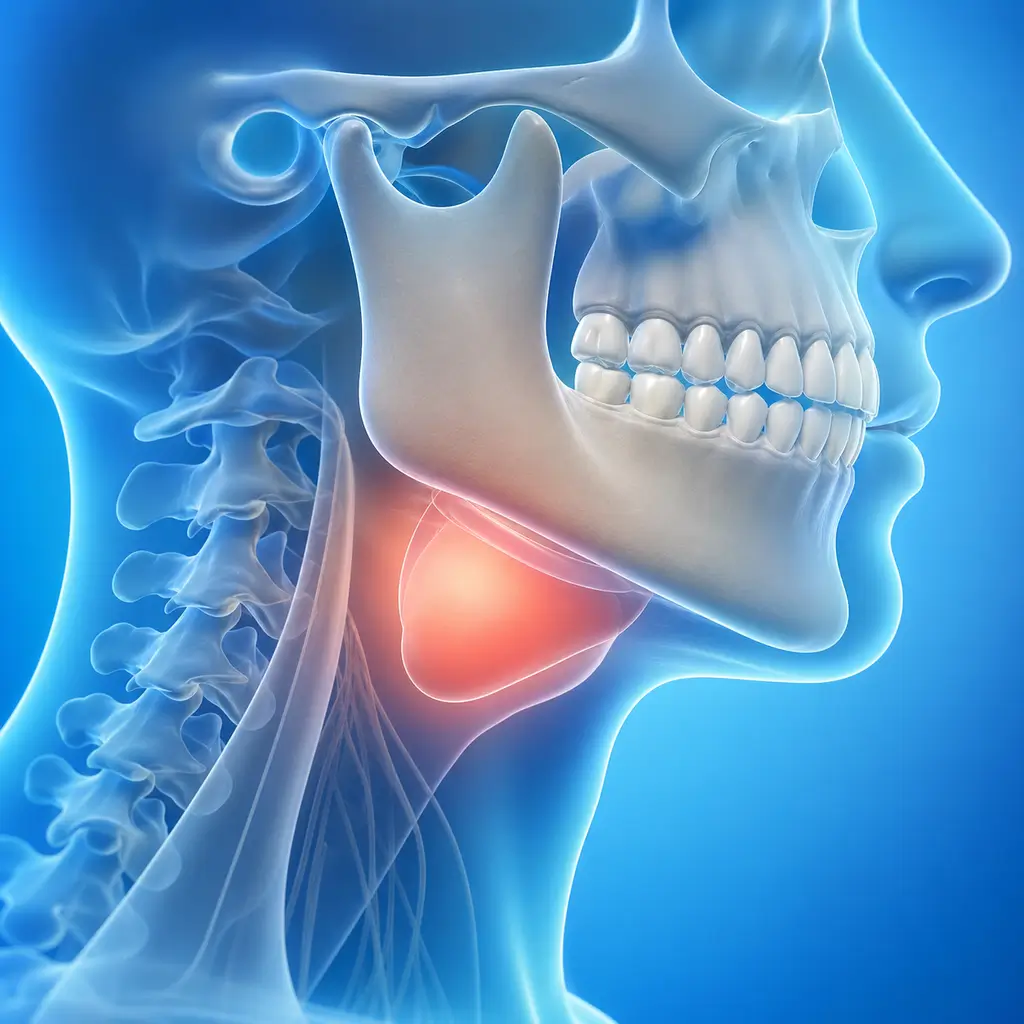
Common Symptoms
Recognizing Maxillofacial space infection
Focus on the most useful decision cues first: common symptoms, the patients or situations that usually prompt review, and any signs that need faster assessment.
Common Symptoms
Signs patients often notice before evaluation
Local signs include redness, swelling, heat, pain, and functional impairment
Systemic symptoms include fever, chills, fatigue, loss of appetite, and headache. Severe cases may show signs of sepsis, such as fast heart rate, rapid breathing, and low blood pressure
When to Seek Evaluation
Typical patients and situations that warrant review
People with a history of odontogenic infection, such as periapical periodontitis, wisdom tooth pericoronitis, or periodontitis, accounting for more than 70%
Patients with diabetes, especially when blood glucose is poorly controlled
Immunocompromised people, such as long-term steroid use, chemotherapy, AIDS, or post-organ transplant
Children, in whom glandular infections such as tonsillitis or lymphadenitis spreading are more common
Unexplained maxillofacial swelling, pain, or fever
Facial swelling after toothache, especially with limited mouth opening
Rapidly spreading facial swelling with high fever and chills
Swallowing difficulty, hoarseness, or breathing difficulty
Floor-of-mouth swelling with tongue elevation and drooling
Fluctuation in the maxillofacial area, suggesting abscess formation
Urgent Assessment
If breathing difficulty, stridor, floor-of-mouth swelling with tongue elevation, high fever and chills, fast heart rate, low blood pressure, facial swelling enlarging within hours, swallowing difficulty, inability to eat, severe limited mouth opening, or altered consciousness occurs, seek emergency care immediately because airway compression and sepsis are possible.
Treatment Approaches
Treatment Directions for Maxillofacial space infection
Treatment follows the principles of effective anti-infective therapy, adequate drainage, removal of the cause, and systemic support, and requires urgent management
Conservative treatment, used for early infection without abscess and mild systemic symptoms, includes systemic antibiotics, symptomatic supportive treatment such as fever control, fluid replacement, and nutrition support, and control of underlying disease, especially diabetes
Surgical treatment, used when an abscess has formed, conservative treatment is ineffective after 24-48 hours, or breathing difficulty or sepsis signs occur, includes incision and drainage at the most fluctuant or dependent site, blunt dissection into the abscess cavity, thorough pus drainage, and drain placement
Remove the cause, such as extraction of the source tooth, curettage of a periapical lesion, or treatment of pericoronitis
If airway compression or breathing difficulty occurs, tracheotomy or tracheal intubation is performed, and severe cases require ICU monitoring
What usually shapes the treatment plan
Clinical Assessment
Key Assessments for Maxillofacial space infection
These are the main areas doctors usually review first. If you already have relevant test or imaging reports, bring them to speed up the assessment. They are helpful but not required, and the same workup can also be completed in China.
Airway assessment: whether breathing difficulty is present
Stridor
Floor-of-mouth swelling
Tongue elevation, ability to lie flat, and suffocation risk
Systemic assessment: vital signs, including temperature, heart rate, respiratory rate, blood pressure, and oxygen saturation, and signs of sepsis or septic shock
Local infection assessment: infection site, including which space or spaces are involved
Swelling extent
Whether fluctuation is present, suggesting abscess formation
Skin color and tension
Mouth opening
Systemic complications, such as mediastinitis
Pericarditis
Brain abscess
Sepsis
Infection source assessment: odontogenic, glandular, traumatic, or hematogenous
Underlying diseases: diabetes
Immunodeficiency
Coagulation disorders
Liver and kidney function
Before You Travel
How to Prepare
Bring previous systemic disease and dental treatment records, and recent imaging and laboratory results if available
Planning Notes
Pre-Assessment Required
An oral specialist should perform an intraoral examination and, as appropriate, periodontal probing, pulp vitality testing, periapical radiographs, panoramic radiographs, or CBCT before determining the treatment plan. Key checks include clinical examination of the infection site, involved spaces, swelling extent, fluctuation suggesting abscess, skin color and tension, mouth opening, and infection source such as source tooth or lymphadenitis; laboratory tests including complete blood count to assess infection severity, pus culture and susceptibility testing to guide antibiotics, blood glucose and HbA1c to assess diabetes, and liver and kidney function and electrolytes to assess overall status and medication safety; and imaging, especially maxillofacial CT to identify involved spaces, abscess extent, foreign bodies, bone destruction, and downward spread to the neck or mediastinum, with neck and chest CT added if needed. Bring clinical examination information, maxillofacial CT, blood count, CRP, procalcitonin, blood glucose, and HbA1c if available.
Remote Pre-Assessment
Intraoral photos, the course of pain/swelling, previous dental records, and imaging can be submitted remotely for preliminary triage, urgency assessment, and an estimated treatment direction. Final diagnosis still requires in-person intraoral examination and necessary imaging.
Multidisciplinary Assessment
Depending on the condition, joint evaluation by oral and maxillofacial surgery, endodontics, periodontics, prosthodontics, orthodontics, imaging, anesthesia, or other related disciplines is recommended, especially for complex infection, tumors, trauma, jaw lesions, or high systemic disease risk.
Medical History Important
Previous dental treatment history, imaging, allergy history, anticoagulant/bisphosphonate use, diabetes, and immune-related diseases can affect diagnosis, anesthesia, bleeding and infection risk, and treatment selection.
Ready to Explore Treatment for Maxillofacial space infection?
Let Carevia help you connect with the right specialists, compare hospitals, and plan your medical trip to China.