Cataract
A common eye condition where the natural lens becomes cloudy, causing progressive vision loss. When vision is meaningfully affected, surgery is the main effective way to restore visual function.
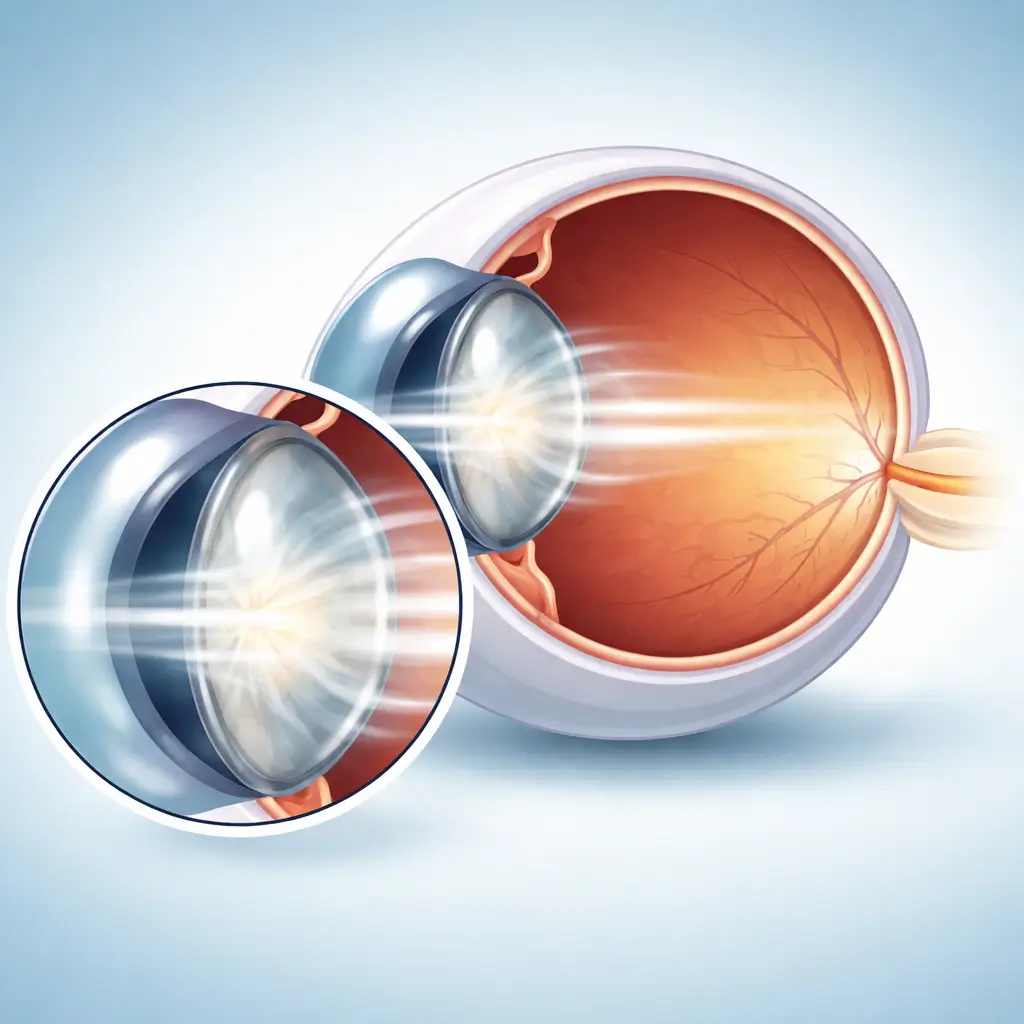
Common Symptoms
Recognizing Cataract
Focus on the most useful decision cues first: common symptoms, the patients or situations that usually prompt review, and any signs that need faster assessment.
Common Symptoms
Signs patients often notice before evaluation
Gradual blurring of vision, like looking through frosted glass
Glare sensitivity, worse vision in bright light
Significantly reduced night vision
Colors appearing yellowish or faded
Sudden increase in nearsightedness (nuclear cataract)
Double vision in one eye
When to Seek Evaluation
Typical patients and situations that warrant review
Adults over 60 (incidence increases significantly with age)
Diabetes patients
Long-term corticosteroid users
History of eye trauma or previous eye surgery
High myopia patients
Individuals with prolonged UV exposure
Vision loss affecting daily activities such as reading, driving, or watching TV
Unable to achieve satisfactory vision correction with glasses
Lens opacity detected during routine eye examination
Treatment Approaches
Treatment Directions for Cataract
No proven medication can reverse cataract progression; when visual function is affected, surgery is the main treatment
Phacoemulsification with IOL implantation is the standard procedure
Monofocal, toric, or selected presbyopia-correcting IOL options may be chosen based on patient needs
In carefully selected patients, trifocal or other presbyopia-correcting IOLs can reduce dependence on glasses across distance, intermediate, and near tasks
What usually shapes the treatment plan
Clinical Assessment
Key Assessments for Cataract
These are the main areas doctors usually review first. If you already have relevant test or imaging reports, bring them to speed up the assessment. They are helpful but not required, and the same workup can also be completed in China.
Best corrected visual acuity test
Slit-lamp examination (assess lens opacity type and severity)
Dilated fundus examination (rule out retinal conditions)
Axial length and corneal curvature measurement (IOL power calculation)
Corneal endothelial cell count
Intraocular pressure measurement
Before You Travel
How to Prepare
Bring recent refraction reports and previous eye examination records
Prepare a complete medical history list (especially diabetes, hypertension)
List all current medications (including anticoagulants)
If the hospital has a perioperative drop protocol, use the prescribed preoperative eye drops as directed
No eye makeup on the day of surgery
Planning Notes
Pre-Assessment Required
A comprehensive preoperative eye examination is required, including visual acuity, intraocular pressure, corneal topography, axial length measurement, corneal endothelial cell count, and dilated fundus exam. These determine surgical suitability and enable precise IOL power calculation. Systemic health screening is also needed to rule out surgical contraindications.
Remote Pre-Assessment
Recent eye examination reports, visual acuity records, and systemic health reports can be submitted remotely for preliminary evaluation. The doctor can provide initial assessment of surgical suitability and IOL recommendations, but the final plan requires in-person precision instrument measurements.
Multidisciplinary Assessment
Medical History Important
Diabetes control directly affects surgical timing and postoperative recovery; anticoagulant use requires advance assessment for possible discontinuation; previous eye surgery history influences the surgical approach.
Ready to Explore Treatment for Cataract?
Let Carevia help you connect with the right specialists, compare hospitals, and plan your medical trip to China.