Selective Laser Trabeculoplasty (SLT)
A frequency-doubled Nd:YAG laser selectively targets pigmented trabecular meshwork cells to enhance aqueous outflow and safely lower intraocular pressure in glaucoma — a repeatable, non-incisional procedure.
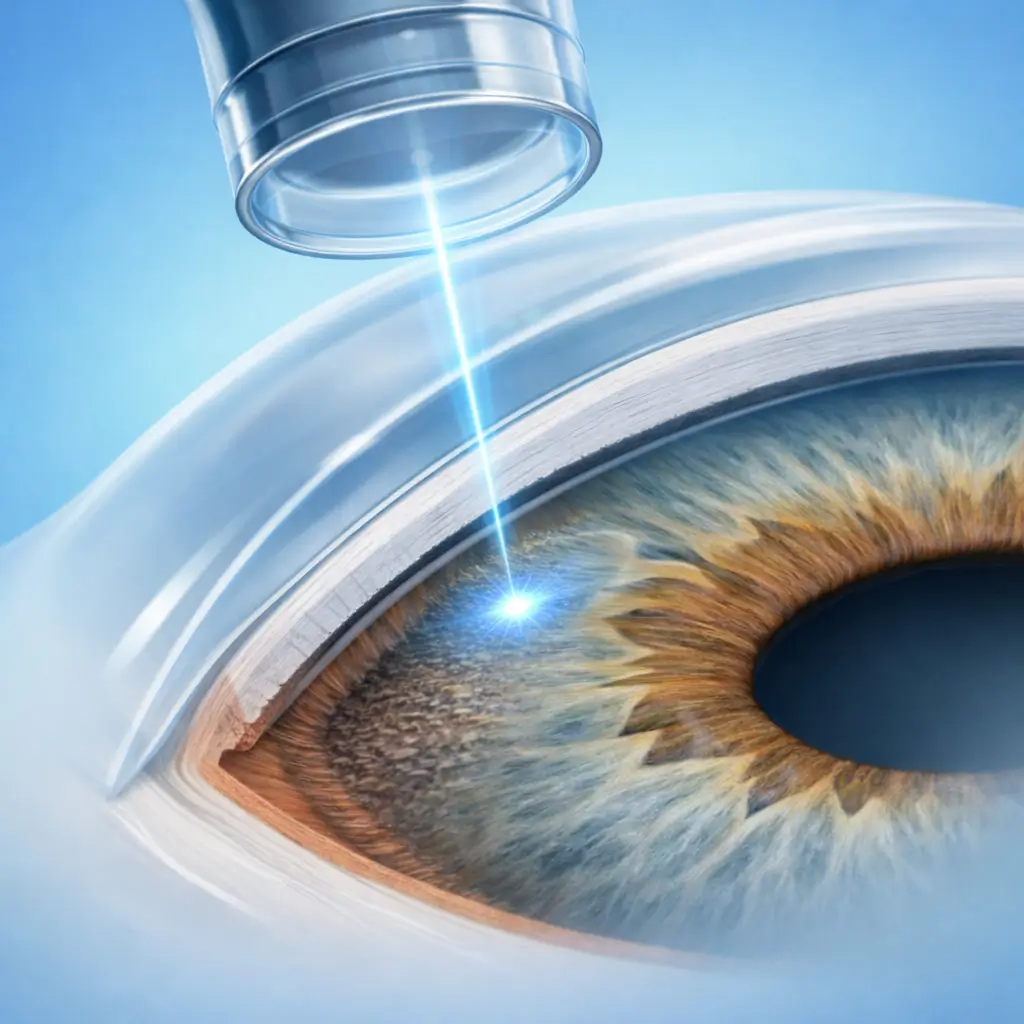
Selective Laser Trabeculoplasty (SLT) is a first-line laser intervention for open-angle glaucoma. The 532 nm frequency-doubled Nd:YAG laser exploits selective photothermolysis to target pigmented cells within the trabecular meshwork, triggering a biological cascade of cytokine release and macrophage infiltration that improves aqueous outflow facility and lowers IOP. Because each laser pulse is only 3 nanoseconds long, thermal diffusion is negligible; surrounding non-pigmented cells and trabecular architecture are preserved. This distinguishes SLT from traditional argon laser trabeculoplasty (ALT) — SLT causes less collateral damage and can be repeated. SLT typically reduces IOP by 20-30%. Effect onset is approximately 4-6 weeks post-treatment, and duration varies considerably (1-5 years). When the effect wanes, SLT can be repeated, which is its main advantage over ALT. SLT may serve as first-line therapy replacing topical IOP-lowering drops (supported by several major guidelines) or as adjunctive treatment when medications are inadequate, deferring or avoiding incisional surgery. The procedure is performed at the slit lamp using a goniolens and requires no hospitalization, making it one of the most accessible interventions for glaucoma management.
Quick Reference
Treatment
10 mins – 20 mins
Observation
1 hours – 2 hours
Est. Cost
¥658.41 – ¥2,633.63
Department
Ophthalmology
Who Is This For
Is Selective Laser Trabeculoplasty (SLT) Right for You?
Good Candidates
- Primary open-angle glaucoma (POAG) and ocular hypertension
- Inadequate IOP control on medical therapy, or intolerance/side-effects to glaucoma drops
- Adherence difficulties with daily eye drop regimens
- Pseudoexfoliative glaucoma (often shows a greater pressure response)
- Moderate IOP elevation (22-35 mmHg) with adequate trabecular pigmentation
May Not Be Suitable
- Closed-angle glaucoma (angle closure prevents laser access to the trabecular meshwork)
- Neovascular glaucoma (fibrovascular membrane covers the trabecular meshwork)
- Prior maximal-dose ALT (full 360° treatment) that has already failed
- Corneal opacity obscuring the laser path or gonioscopic view
- Active uveitic glaucoma (active intraocular inflammation is a contraindication)
Step-by-Step Process
How Selective Laser Trabeculoplasty (SLT) Works
Preparation and Topical Anesthesia
The patient is seated at the slit lamp. Topical anesthetic drops and a prophylactic alpha-agonist (brimonidine) are instilled to reduce post-laser IOP spikes. A goniolens coupled with methylcellulose is placed on the cornea.
Angle Visualization and Parameter Selection
The trabecular meshwork is visualized through the goniolens. The pigmentation grade (0-4) is assessed to guide energy selection (typically starting at 0.8-1.0 mJ, adjusted to the threshold producing a subtle champagne bubble without excessive tissue response).
Laser Application
Approximately 50-100 non-overlapping laser spots are placed evenly across 180° or 360° of the trabecular meshwork (25-50 spots per quadrant). Each spot is monitored for an appropriate tissue response; over-treatment is avoided.
Post-Laser IOP Check and Discharge
The goniolens is removed and the cornea rinsed. IOP is measured 30-60 minutes later to rule out an acute pressure spike (incidence ~5%). Once IOP is confirmed stable, a topical anti-inflammatory drop prescription is provided and the patient is discharged.
SLT is typically completed in a single session covering 180° or 360° of the trabecular meshwork. IOP reduction becomes apparent at 4-6 weeks and persists for 1-5 years on average. The procedure may be repeated when the effect diminishes.
Cost Information
Cost Estimate for Selective Laser Trabeculoplasty (SLT)
Estimated Price Range
¥658.41 – ¥2,633.63
What's Included
Public tier-3A International Medical Department: approximately ¥4,500-9,000 (180° or 360°); premium private eye centers: approximately ¥10,000-18,000, typically including comprehensive preoperative assessment, laser treatment, and follow-up package.
Before Your Visit
What to Prepare
Required Tests & Examinations
If you already have recent valid test results, bring the reports. If not, these assessments can usually be completed in China before the procedure.
IOP measurement (baseline pressure and treatment target)
Gonioscopy (assess angle width and trabecular meshwork pigmentation grade — determines laser feasibility)
Visual field testing (Humphrey perimetry — document baseline function)
Optic nerve OCT (document baseline structural status)
Central corneal thickness (CCT correction affects true IOP interpretation)
Documents & Materials to Bring
Required to Bring
Glaucoma diagnosis records and complete current medication list
Recent IOP measurement log
Visual field and optic nerve OCT reports
Passport and valid visa
After Treatment
Recovery & Follow-Up
Mild redness and foreign-body sensation on the day of treatment are normal and usually resolve within 1-2 days
Use prescribed topical NSAID drops for 3-5 days to reduce postoperative inflammation
Do not discontinue existing IOP-lowering drops until the doctor confirms adequate effect at the follow-up visit
At the 4-6 week follow-up, the physician will assess whether medications can be reduced or stopped
Contact the clinic promptly if significant eye pain or vision loss occurs — rule out acute IOP elevation
Follow-Up Schedule
IOP check 1-2 hours post-procedure (rule out acute pressure spike); efficacy evaluation at 4-6 weeks (adjust medications as needed); routine follow-up every 3-6 months thereafter.
Related Conditions
Conditions This Procedure Treats
Ready to Plan Selective Laser Trabeculoplasty (SLT) in China?
Let Carevia help you find the right hospital, coordinate your treatment, and arrange every detail of your medical trip.
Frequently Asked Questions
Need personalized guidance?
Our care coordinators can help you assess whether this procedure fits your situation.
Contact Us