Impacted tooth
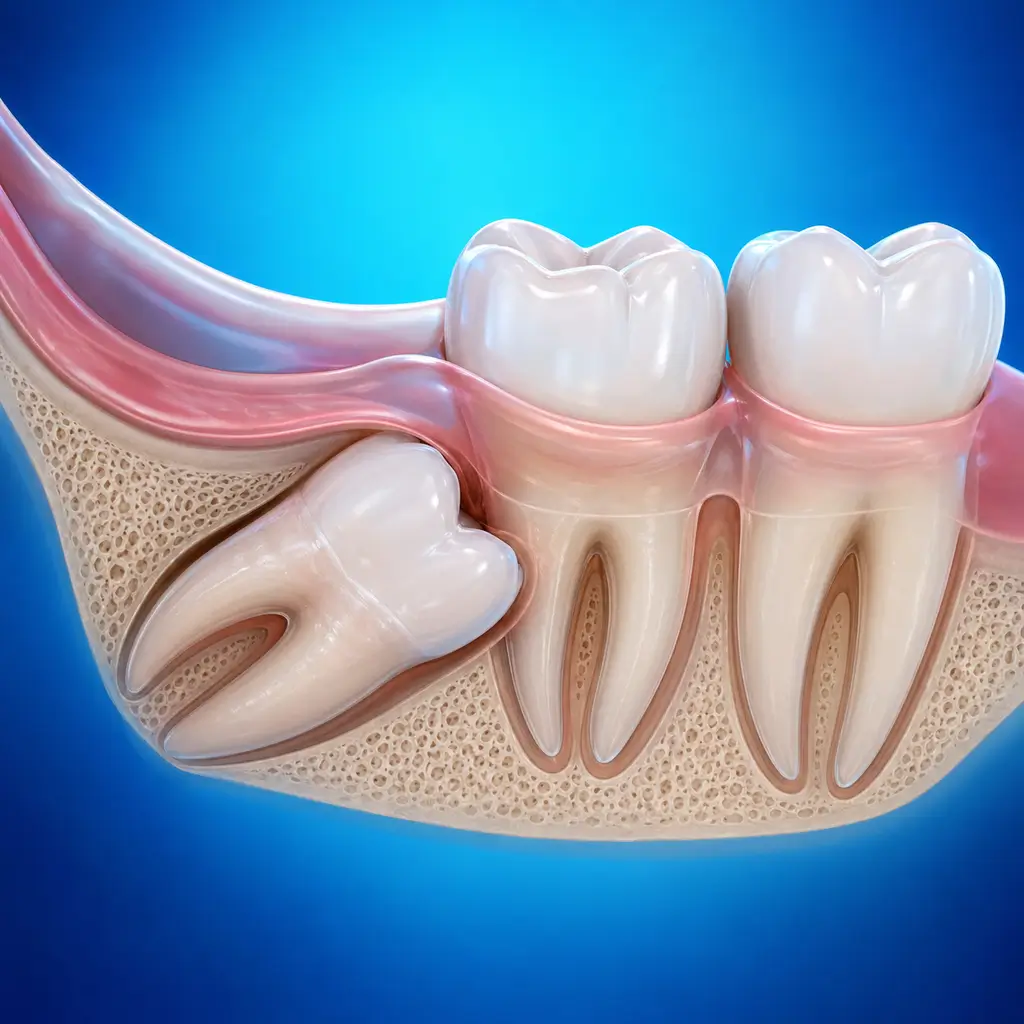
A tooth that cannot erupt normally and remains within bone or soft tissue. It may be asymptomatic or cause pericoronitis, damage to adjacent teeth, or cysts.
Common Symptoms
Recognizing Impacted tooth
Focus on the most useful decision cues first: common symptoms, the patients or situations that usually prompt review, and any signs that need faster assessment.
Common Symptoms
Signs patients often notice before evaluation
The tooth is partially erupted or not erupted at all, with part or all of it covered by gingiva
Repeated pericoronitis with local swelling and pain, limited mouth opening, pus discharge, and facial swelling
Pressure from the impacted tooth causes adjacent tooth mobility, caries, or pulpitis
Food impaction between the impacted and adjacent teeth, with bacterial breakdown causing bad breath
Asymptomatic: most impacted teeth cause no subjective symptoms early and are found only on radiographs
When to Seek Evaluation
Typical patients and situations that warrant review
Common in young and middle-aged adults
A tooth has not erupted beyond the normal eruption time while the contralateral same tooth has erupted
Repeated wisdom tooth pericoronitis
Impacted tooth causes adjacent tooth pain, mobility, or caries
Orthodontic treatment requires removal of an impacted tooth to provide space or prevent relapse
Treatment Approaches
Treatment Directions for Impacted tooth
Impacted teeth that have caused pericoronitis, adjacent tooth damage, cysts, or are needed for orthodontic reasons should be extracted electively
Deeply positioned impacted teeth without complications and without eruption potential, such as completely bony impacted teeth not affecting adjacent teeth, may be observed regularly
For impacted maxillary canines and other teeth important for function and esthetics, orthodontic treatment may use surgical exposure plus orthodontic traction to preserve the tooth and guide eruption into the normal position
What usually shapes the treatment plan
Clinical Assessment
Key Assessments for Impacted tooth
These are the main areas doctors usually review first. If you already have relevant test or imaging reports, bring them to speed up the assessment. They are helpful but not required, and the same workup can also be completed in China.
Position of the impacted tooth and relationship to adjacent teeth
Relationship to important anatomical structures, such as the mandibular nerve canal, maxillary sinus, and adjacent tooth roots
Whether dentigerous cysts or other lesions are present
Presence of symptoms and complications
Patient age and systemic condition
Before You Travel
How to Prepare
Bring previous imaging records
Planning Notes
Pre-Assessment Required
An oral specialist should perform an intraoral examination and, as appropriate, periodontal probing, pulp vitality testing, periapical radiographs, panoramic radiographs, or CBCT before determining the treatment plan. Key checks include visual assessment of eruption, gingival flap coverage, redness, swelling, and pus discharge; probing pocket depth and checking adjacent teeth for caries or mobility; percussion to assess adjacent tooth pulpitis; and imaging to clarify impacted tooth morphology and position. Bring oral examination and imaging records if available.
Remote Pre-Assessment
Intraoral photos, the course of pain/swelling, previous dental records, and imaging can be submitted remotely for preliminary triage, urgency assessment, and an estimated treatment direction. Final diagnosis still requires in-person intraoral examination and necessary imaging.
Multidisciplinary Assessment
Medical History Important
Previous dental treatment history, imaging, allergy history, anticoagulant/bisphosphonate use, diabetes, and immune-related diseases can affect diagnosis, anesthesia, bleeding and infection risk, and treatment selection.
Ready to Explore Treatment for Impacted tooth?
Let Carevia help you connect with the right specialists, compare hospitals, and plan your medical trip to China.